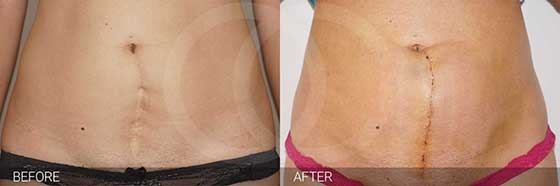
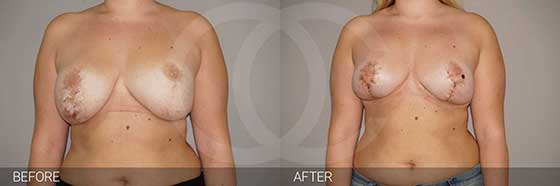
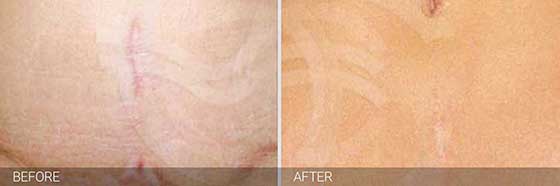
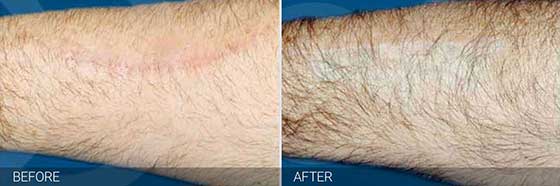
Got a Scar You Hate? You Don’t Have to Live with It
Scarring can have a big impact on your wellbeing - not only can scars detract from your appearance, but they can also remind you of trauma you’d rather forget.
You might think there’s nothing you can do about scars. After all, you might have got them as a result of previous surgery. But scar correction surgery can often work wonders in reducing the size of a scar, smoothing out the texture and making it much neater and less noticeable.
Scar correction can also help in cases where the skin has healed in such a way that it is restricting movement or causing pain. And it’s also suitable for burn scars and deep acne scars.
Director of Ocean Clinic Group Dr Kai Kaye is a specialist in scar revision, having trained in this field at the Plastic and Reconstructive Surgery Department at the University of Aachen in Germany. Read on to find out what causes bad scars and what can be done to correct them
Why do I have a bad scar?
Scarring can turn out badly for a number of reasons. Factors that influence how well you heal include:
- Your skin type - some people simply scar worse than others. Darker skin is more prone to make the worst scars and people with very pale skin can also be poor scar makers.
- The location of the scar - if it’s along a joint, on skin which has a lot of movement (on a knee, for example) the scarring will be worse than if it’s on skin that doesn’t move (like behind the ear).
- The suture technique - if your wound is not stitched up well - or you fail to get medical attention for a wound - it can result in uneven healing.
- Your aftercare - if you fail to look after your scar during the healing process, for example by exposing it to UV light, it can become discoloured.
Types of scars
Beyond normal, fine-line scars, there are four different types of scars that can result in a less than optimal healing outcome. These are:
Keloid scars
A keloid scar is one that’s raised, often red, and goes beyond the boundaries of the original wound. They’re caused by an overgrowth of tissue that happens when too much collagen is produced at the site of a wound. Some people are prone to keloid scarring, especially people with more pigment in their skin. In these individuals, even a simple insect bite can end up in a significant scar. Keloid scars are often itchy or painful and can restrict movement if they’re near a joint.
Hypertrophic scars
Like keloid scars, hypertrophic scars are ones that rise above the surface of the skin, however, they do not extend beyond the boundary of the original wound. They’re also the result of an imbalance in collagen at the site of the wound. Hypertrophic scars occur when there is a lot of tension around a healing wound. They may continue to thicken for up to 6 months before gradually improving over a few years.
Atrophic scars
These are pitted or sunken scars caused by a bad case of acne or chickenpox. They can also develop as a result of an injury that causes a loss of underlying fat. Atrophic scars stay within the boundary of the original wound and typically occur in the face or on the back.
Scar contractures
Scar contractures are tight scars that occur on a joint. They’re often caused by burns and happen when the skin "shrinks" and pulls on the surrounding tissue. This restricts movement of the joint, which can also make them painful.
What’s a ‘good’ scar?
A ‘good’ scar is one that fades to be a barely noticeable fine line that blends in with the surrounding skin tone. It should be placed in the right direction to ensure there is not too much tension exerted on the scar. Wherever possible, the scar should be hidden in the natural folds of the skin, for example beneath the breast or in the groin.
Experienced surgeons can influence the result through meticulous technique and by using dissolving sutures or glue and removing other stitches early enough to avoid stitch marks. What’s more, proper aftercare - such as using silicone sheets - will ensure the best results.
How a bad scar is repaired
If you have a scar that is causing you problems or you consider ugly there are various options available to you. In addition to surgical excision, there are non-surgical treatments that can improve the appearance of a scar. Usually, the best results can be achieved through a combination of surgery and non-invasive procedures.
Surgical correction
Scar excision
In simple terms, scar excision is cutting out the existing scar and resealing the wound. But there are a number of different excision techniques a surgeon can use depending on the type of scar you have. For example, extramarginal scar excision involves excision of a small margin of the normal skin along with the scar in order to get normal tissue at the wound margins. On the other hand, intramarginal scar excision is done by cutting away portions of the scar at intervals of 6-12 weeks in order to preserve the normal skin as much as possible.
Tissue expansion
This is a procedure performed to promote the growth of healthy supplementary skin used for the replacement of damaged skin. It’s carried out by placing a balloon-like expander underneath the skin near the damaged region. Over time, the expander is filled with saline (or saltwater) solution causing the skin around it to stretch and grow. Once the new skin has reached its ideal size the tissue expander is removed and the new skin is redistributed, replacing the damaged area of skin. Often, tissue expansion is done before reconstructive burn surgery, using the new skin to replace scar tissue at the burn injury site.
Skin flaps
A skin flap is healthy skin and tissue that is partly detached and moved to cover a nearby wound. Flaps are transferred with their own, original blood supply (pedicle flap) and can be ‘local’ or ‘regional’. Local flaps are flaps that are located adjacent to the scar site. Regional flaps are located at a distance from the donor site and are used for extensively burned contractures on movable areas such as the anterior neck. Sometimes a flap is moved to a new site and the blood vessels are surgically reconnected. This is called a ‘free’ flap.
Skin graft
A skin graft involves removing skin from one area of the body and moving it (without its blood supply) to another. Skin grafts survive as oxygen and nutrients diffuse into them from the underlying wound bed. A ‘split-thickness’ graft involves removing the top layer of the skin (the epidermis) as well as a portion of the deeper layer of the skin, called the dermis, usually harvested from the front or outer thigh, abdomen, buttocks, or back. Split-thickness grafts are used to cover large areas. ‘Full-thickness’ grafts involve removing all of the epidermis and dermis from the donor site. These are usually taken from the abdomen, groin or forearm and are used for small wounds on highly visible parts of the body, such as the face.
Fat graft
Fat grafting involves the extraction of fat from a donor site on the body (such as the tummy). It’s then processed and used to restore volume under depressed or adherent scars. Because fat tissue is rich in growth factors and stem cells it also results in skin regeneration, with excellent results for scar correction.
Non-surgical correction
Steroid injections
Especially effective in keloid scars and hypertrophic scars, steroids are injected directly into the scar tissue to help decrease the itching, redness, and burning sensations that these scars may produce. The injections also help to decrease the size of the scar and soften the scar tissue. Injections are repeated over a 3-6 months period, resulting in progressive improvement.
Laser resurfacing
Laser resurfacing uses high-energy light to burn away damaged skin. Lasers may be used to smooth a scar, remove the abnormal colour of a scar, or flatten a scar.
Dermabrasion
Dermabrasion involves removing the top layers of skin with an electrical machine that abrades the skin. As the skin heals from the procedure, the surface appears smoother and fresher. It’s a useful treatment for small surgical scars and acne scars.
Chemical peels
Chemical peels offer another method for resurfacing the skin. A chemical solution is applied to dissolve the top layer of skin. This triggers the skin to regenerate, often improving the appearance of superficial scars and correcting irregular colour.
Microneedling
Tiny needles are used to create micro-injuries to the inner and outer layers of the scar tissue, triggering the body’s healing process. By encouraging the production of new collagen and elastin, microneedling improves the texture of the scar. The channels created by the needles can also be used for the deep delivery of topical creams.
Ultrasound treatment
Ultherapy is an ultrasound treatment used to stimulate collagen and elastin. It does this by heating the layers beneath the skin and creating thermal microtrauma - this leads to a reformation of elastic fibres and improves the appearance of scars.
Hyaluronic acid filler
To fill atrophic scars (sunken or pitted), Radiesse, an injectable filler can be used. The filler is diluted (mixed with saline and lidocaine to thin it out) and injected superficially. As well as adding volume and making the surface of the scar smoother, it can help to improve discolouration.
Downtime and aftercare
In most cases, scar correction treatment can be done on an outpatient basis and requires little to no downtime. Only when extensive skin grafting is required do patients need to stay overnight in the clinic.
To achieve the best possible results, all our scar correction treatments include advanced scar care dressings. Silicone sheets and patches are important tools as they help to soften and decrease the redness of scars.
We also provide compression garments to wear over the treated area and apply pressure to the scar. Especially useful in the treatment of burn scars, pressure therapy may be applied continuously for many months in order to avoid the scar elevating above the surrounding skin level and to reduce itching, redness and swelling.
Would you like to know how the appearance of your scar could be improved? Let us take a look. We offer both in-clinic and online consultations. Contact Ocean Clinic to book.